PubMed Central, CAS, DOAJ, KCI

Articles
- Page Path
- HOME > J Yeungnam Med Sci > Volume 39(3); 2022 > Article
-
Image vignette
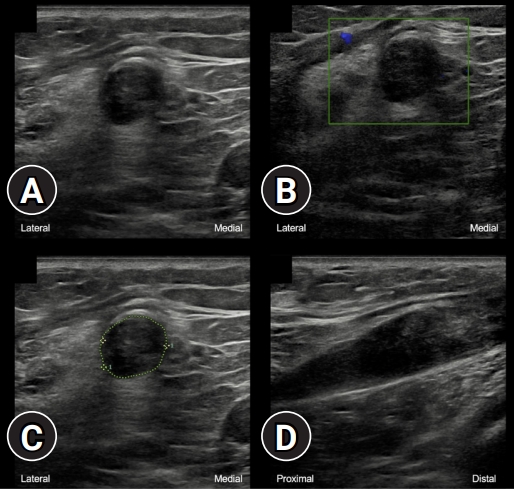
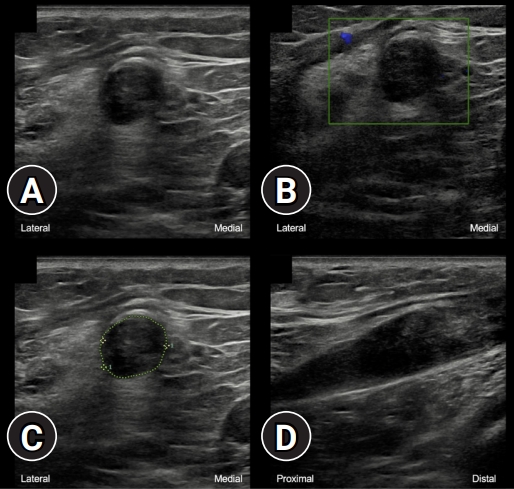
Playing snakes and ladders with the common fibular nerve on ultrasound after knee dislocation -
Natan Bensoussan
 , Mathieu Boudier-Revéret
, Mathieu Boudier-Revéret , Johan Michaud
, Johan Michaud
-
Journal of Yeungnam Medical Science 2022;39(3):266-267.
DOI: https://doi.org/10.12701/yujm.2021.01389
Published online: September 15, 2021
Department of Physical Medicine and Rehabilitation, Centre hospitalier de l'Université de Montréal, Montréal, QC, Canada
- Corresponding author: Mathieu Boudier-Revéret, MD Hôtel-Dieu du Centre hospitalier de l'Université de Montréal, 3840 rue Saint-Urbain, Montréal, QC, H2W 1T8, Canada Tel : +1-514-890-8000 Fax: +1-514-412-7610 E-mail: mathieu.boudier-reveret@umontreal.ca
Copyright © 2022 Yeungnam University College of Medicine, Yeungnam University Institute of Medical Science
This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License (http://creativecommons.org/licenses/by-nc/4.0/) which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
- 3,620 Views
- 87 Download
Supplementary material
-
Ethical statements
Written patient consent was obtained.
-
Conflicts of interest
No potential conflict of interest relevant to this article was reported.
-
Funding
None.
-
Author contributions
Conceptualization: all authors; Writing-original draft: NB, MBR; Writing-review & editing, Validation: all authors.
Notes
- 1. Coraci D, Tsukamoto H, Granata G, Briani C, Santilli V, Padua L. Fibular nerve damage in knee dislocation: Spectrum of ultrasound patterns. Muscle Nerve 2015;51:859–63.ArticlePubMed
- 2. Bonnevialle P, Dubrana F, Galau B, Lustig S, Barbier O, Neyret P, et al. Common peroneal nerve palsy complicating knee dislocation and bicruciate ligaments tears. Orthop Traumatol Surg Res 2010;96:64–9.ArticlePubMed
- 3. Morris BL, Grinde AS, Olson H, Brubacher JW, Schroeppel JP, Everist BM. Lariat sign: an MRI finding associated with common peroneal nerve rupture. Radiol Case Rep 2018;13:743–6.ArticlePubMedPMC
References
Figure & Data
References
Citations


 E-Submission
E-Submission Yeungnam University College of Medicine
Yeungnam University College of Medicine PubReader
PubReader ePub Link
ePub Link Cite
Cite