An update on immunotherapy with PD-1 and PD-L1 blockade
Article information
Abstract
Cancer is the leading cause of death and is on the rise worldwide. Until 2010, the development of targeted treatment was mainly focused on the growth mechanisms of cancer. Since then, drugs with mechanisms related to tumor immunity, especially immune checkpoint inhibitors, have proven effective, and most pharmaceutical companies are striving to develop related drugs. Programmed cell death-1 and programmed cell death ligand-1 inhibitors have shown great success in various cancer types. They showed durable and sustainable responses and were approved by the U.S. Food and Drug Administration. However, the response to inhibitors showed low percentages of cancer patients; 15% to 20%. Therefore, combination strategies with immunotherapy and conventional treatments were used to overcome the low response rate. Studies on combination therapy have typically reported improvements in the response rate and efficacy in several cancers, including non-small cell lung cancer, small cell lung cancer, breast cancer, and urogenital cancers. The combination of chemotherapy or targeted agents with immunotherapy is one of the leading pathways for cancer treatment.
Introduction
Cancer, the leading cause of death, is on the rise worldwide. According to recently published cancer statistics in Korea in 2018, the growing trend in cancer incidence has slowed compared to 2014, but it can be found that the cancer incidence rate continues to increase until then [1]. Accordingly, there has been a large body of research and progress on gene mutations related to cancer growth and the development of targeted treatments. Until 2010, the development of targeted treatment was mainly focused on cancer’s growth mechanism. However, since then, drugs with mechanisms related to tumor immunity, especially immune checkpoint inhibitors (ICIs), have proven effective [2], and almost all pharmaceutical companies are striving to develop related drugs.
Tumor immunotherapy refers to cancer treatment using the human immune system. Over the past century, cancer researchers have conducted extensive research to treat cancer by strengthening the mechanism by which human immunity recognizes and fights against tumor cells. However, immunotherapy has limitations in its effectiveness and is a structure that strengthens immune-related mechanisms; therefore, it often causes serious side effects, leading to skepticism about tumor immunotherapy among oncologists [3]. However, since 2010, surprising results of tumor immunotherapy, especially monoclonal antibodies related to ICIs, have been reported [4]. Thus, monoclonal antibodies related to ICIs are emerging as a new alternative to metastatic cancer treatment.
Tumor immunotherapy includes not only allogeneic bone marrow transplantation, which has been used for a long time, but it covers various treatment modalities, including tumor vaccines, cytokines, monoclonal antibodies, adoptive cell therapy, and cell therapy. In this article, we review programmed death-1 (PD-1) and programmed death ligand-1 (PD-L1) inhibitors, which are ICIs that are widely applied in clinical practice.
Mechanism of PD-1 and PD-L1
To explain the mechanism of PD-1 and PD-L1, we first discuss the immune cells in the body, especially the T cell lymphocyte immune reaction mechanism. Controlling T cell lymphocyte immune reaction is both complex and precise. For activating T lymphocytes, in advance, the action started with antigen recognition of T cells by binding antigen-bound antigen-presenting cells (APCs) at the T-cell antigen receptor [5]. To fully activate T cells, a stimulatory signal, in which CD80, CD40 expressed on APC surfaces bind the ligand on the T lymphocytes’ surface including CD28, CD40 ligand, was needed. Simultaneously, the inhibitory signal is activated to inactivate the activated T-lymphocyte cells after some time to protect against cell damage resulting from excessive immune reactions [6]. The most recognized inhibitory signals are cytotoxic T-lymphocyte antigen (CTLA)-4, PD-1 expressed on T lymphocytes [7]. In particular, PD-1 is known to regulate the function of T lymphocytes in peripheral tissues by binding ligands of PD-L1 or PD-L2 and PD-1 of T lymphocytes [8]. The immune system of the human body plays a role in the recognition and eradication of mutated tumor cells, but it can also promote tumor growth by selecting tumor cells that can evade immune surveillance [9]. Thus, tumor cells acquire the ability to not eradicate tumor cells by antigen recognition of the immune system.
Moreover, tumor cells that escape the immune system can induce an immunosuppressive status by producing cytokines and growth factors, including vascular endothelial growth factor (VEGF), recruiting T cells, and myeloid-derived suppressor cells [5,9,10]. They can also overexpress the inhibitory ligands on their surfaces to escape the immune system and effectively eradicate tumor cells [11,12]. The inhibitory ligands expressed on tumor cells include PD-L1, as mentioned above. PD-L1 is expressed on the tumor cell surface, while PD-1 is expressed on activated B or T lymphocytes [13]. Thus, binding PD-1 ligands on tumor cells at the PD-1 receptor on lymphocytes prevents the activation of immune cells and maintains the progression without eradication by the immune system, preventing the identification of non-self antigens [14].
PD-L1 is frequently found in various human cancers, including melanoma, lung cancer, renal cell cancer (RCC), head and neck cancer, bladder cancer, ovarian cancer, and gastrointestinal cancer [15]. PD-1 inhibitors or PD-L1 inhibitors prevent the binding of inhibitory signals and sustain the function of eradicating tumor cells by maintaining the activation of T lymphocytes [16]. As a result of studies based on human immune mechanisms on tumor cells, in 2010, a PD-1 inhibitor, pembrolizumab, was developed for melanoma treatment for the first time [2], and the other successful results of various cancers in pembrolizumab and nivolumab led to a new chapter in cancer treatment in current days.
PD-1 and PD-L1 inhibitors on market: study results and indication
Currently, most multinational pharmaceutical companies have developed PD-1 or PD-L1 inhibitors for the treatment of various tumors. Here, we describe pembrolizumab, nivolumab, and atezolizumab, which are widely used in Korea.
1. Nivolumab
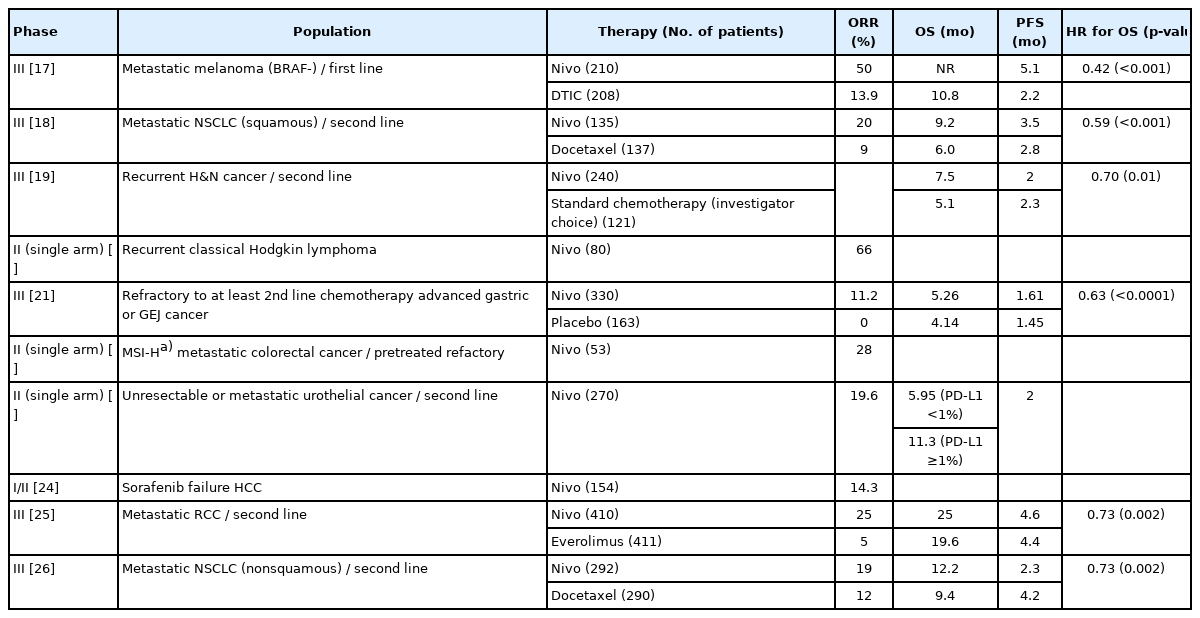
Nivolumab is the first PD-1 inhibitor to be developed to treat refractory metastatic cancers. In December 2014, nivolumab was approved for metastatic or inoperable melanoma by the U.S. Food and Drug Administration (FDA), demonstrating improvement in progression-free survival (PFS) and overall survival (OS) compared to dacarbazine (PFS, 5.1 months vs. 2.2 months; OS, not reached vs. 10.8 months) [17]. Subsequently, showing PFS and OS improvement in the nivolumab group compared to chemotherapy (docetaxel) in metastatic non-small cell lung cancer (NSCLC) second-line treatment [18], nivolumab is gradually expanding and being applied to other cancer types. Currently, its indications are increasing, including malignant melanoma, NSCLC, urothelial cancer, head and neck cancer, hepatocellular cell carcinoma, kidney cancer, Hodgkin’s lymphoma, stomach cancer, and colorectal cancer [19-26] (Table 1).
2. Pembrolizumab
Earlier, the pharmaceutical company developed the CTLA-4 inhibitor, ipilimumab, and tested positive results in melanoma [4]. Subsequently, the PD-1 inhibitor pembrolizumab was used in a phase II study in refractory melanoma patients despite using ipilimumab. The study reported statistically significant results that OS in the pembrolizumab group (2 mg/kg) was improved compared to chemotherapy (13.4 months vs. 11 months) and was approved by FDA [27].
In Korea, pembrolizumab was approved for first-line treatment of inoperable or metastatic melanoma, metastatic NSCLC with first-line treatment, and second-line treatment of NSCLC with PD-L1 expression rate above 50% and absence of epidermal growth factor receptor mutation or ALK rearrangement, which progressed to first-line chemotherapy [28,29]. Its indications are expanding to include Hodgkin’s lymphoma, urothelial cancer, head and neck cancer, and breast cancer [30-34] (Table 2).
3. Atezolizumab
Atezolizumab is a fully-humanized monoclonal antibody against the protein PD-L1, while nivolumab and pembrolizumab are PD-1 inhibitors. Atezolizumab was first approved in advanced urothelial cancer where tumors have progressed after platinum-based chemotherapy by the FDA, showing an improvement in the 12-month OS rate (41%) in a phase 2 study compared to a landmark 12-month OS rate of 20% from an analysis of 10 phase 2 trials who received second-line chemotherapy for advanced urothelial cancer [35] and showed efficacy in platinum-ineligible patients with metastatic urothelial cancer (OS, 15.9 months; PFS, 2.7 months) [36]. Also, atezolizumab was approved by the FDA in palliative second-line treatment of NSCLC showing improvement of OS compared to conventional chemotherapy with docetaxel (OS, 13.8 months vs. 9.5 months; hazard ratio [HR], 0.73; p=0.0003) and metastatic NSCLC which has high expression of PD-L1 first-line treatment by proving the efficacy compared to chemotherapy (OS, 20 months vs. 13.1 months; HR, 0.59; p=0.01) [37,38] (Table 3).
New direction of PD-1 and PD-L1 inhibitors
Although promising results for inhibitors of PD-1 and PD-L1 have been reported, the low response rate of immunotherapy cancer treatment has been reported to be 15% to 20% [39,40]. With the development of immunotherapy leading to PD-1 and PD-L1 inhibitors, efforts to understand tumor immunology last for a better response to immunotherapy. Inflamed tumors that highly infiltrate immune cells and proinflammatory cytokines are known to respond well to immunotherapy. In addition, other immunotherapies, such as CTLA-4 inhibitors, have a better response correlated with posttreatment increases in tumor-infiltrating lymphocytes [41,42]. In other words, an inflamed tumor can have a better response, and immune modulation-induced treatments of weak immunogenic tumors can have similar results, indicating the possibility of therapeutic intervention in immunotherapy. The biomarkers of ICI response have been validated in several studies. Several factors have received much attention, including PD-L1 expression, mutational burden intensity, and deficiencies in antigen presentation [41,43]. PD-L1 expression in tumors was assessed by immunohistochemistry (IHC) staining of PD-L1 positive tumor cells, immune cells, or both cells. High expression PD-L1 in tumors including melanoma, NSLCL, RCC, prostate cancer, and colorectal cancer showed an objective response to nivolumab using a 5% PD-L1 positivity threshold. However, there is a hurdle that multiple variables of PD-L1 IHC staining caused by transient, intrapatient, and intratumoral heterogeneity and poor uniform test of PD-L1 expression result in poor reliability. In addition, as mentioned above regarding the mechanism of PD-1 inhibitors for cancers, neoantigens produced by somatic mutation of tumor cells as primary drivers of anticancer adaptive immune response have been identified in preclinical data. The long-term clinical benefit of high mutational or neoantigen burden with a mutational load of more than 100 nonsynonymous somatic mutations in cancers has been reported in several studies [44,45].
Some modulators act directly on tumors to increase their immunogenicity, including chemotherapy, radiotherapy, and metabolic modifiers. While conventional chemotherapy has a rapid response initially and has been resistant to tumors in a short time, PD-1 or PD-L1 inhibitors have a lower response rate than conventional chemotherapy and sustained the response in the responding group for long periods. To increase the response rate to immunotherapy, combination treatment with immunotherapy was thought to amplify the antitumor immune response (Fig. 1) [46]. In addition, destroying cancer cells by cytotoxic agents release tumor-associated antigens that can stimulate immune responses to infiltrate the immune cells around tumors so that they change to an inflamed tumor [47]. To make an inflamed tumor is essential to increasing the response to PD1 or PD-L1 inhibitors.
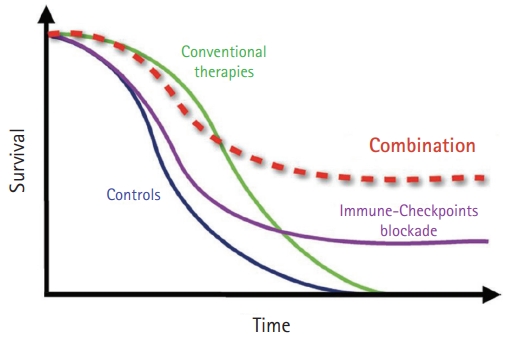
Survival curve of each treatment and expected effect with combination of immune checkpoints blockade with conventional therapies. Combination strategies could show synergistic effects to make appropriate microenvironment enough to play immunotherapy. Adapted from Champiat et al. [46] with permission of Elsevier.
1. Combination of chemotherapy
Recently, many studies have been conducted on combination treatment with immunotherapy, including immunotherapy, chemotherapy, targeted therapy, and radiotherapy. In particular, good candidates with combination treatment are included in chemotherapy or targeted therapy, because conventional therapy could help achieve rapid tumor regression, and immune checkpoint blockade could then help sustain the tumor response, inducing a long-lasting immune-mediated reaction [46]. The study of combination treatment with ICI and chemotherapy started with metastatic NSCLC. In the first-line treatment of metastatic NSLCL, PFS and OS improvement showed the pembrolizumab group with pemetrexed and carboplatin compared to conventional chemotherapy regardless of PD-L1 status (HR, 0.49; p<0.001). In 2018, this combination therapy was first approved by the FDA and is now routinely used as a first-line treatment in metastatic NSCLC [48,49]. Accordingly, the combination of nab-paclitaxel and atezolizumab was recently approved for first-line treatment of triple negative metastatic breast cancer, showing improved OS compared to the nab-paclitaxel only group in PD-L1 positive patients (OS, 25 months vs. 15.5 months) [50]. The PFS of the combination of nab-paclitaxel and atezolizumab group showed the benefit in all populations (7.5 months vs. 5.0 months; HR, 0.62; p<0.001) and failed to show the benefit of OS in all populations. However, this study proved that adding chemotherapy in immunotherapy improved survival benefit in the PD-L1 positive group compared to immunotherapy alone. The great success of combination therapy in NSCLC and breast cancer has led to more studies on combination treatment with immunotherapy. In metastatic small cell lung cancer (SCLC), combination treatment with atezolizumab, etoposide, and carboplatin revealed better survival benefit compared to conventional chemotherapy with etoposide and carboplatin in IMpower 133 study (OS, 12.3 months vs. 10.3 months; HR, 0.70; p=0.007) [51]. Similarly, durvalumab with etoposide and platinum improved the OS compared to conventional chemotherapy in metastatic SCLC first-line treatment in the CASPIAN study (OS months, 13.3 vs. 10.3 months; HR, 0.73; p=0.0047) [52]. In metastatic urothelial cancer, positive results were sustained when reporting the OS improvement of atezolizumab with platinum-containing chemotherapy compared to placebo and platinum-containing chemotherapy in palliative first-line treatment of metastatic urothelial cancer of IMvigor 130 study (PFS: 8.2 months vs. 6.3 months; HR, 0.82; p=0·007; OS: 16 months vs. 13.4 months; HR, 0.83; p=0.027) [53]. However, the OS results were not significant. In addition, the study results of pembrolizumab and platinum-containing chemotherapy vs. pembrolizumab-only vs. chemotherapy only were reported in palliative first-line treatment of metastatic urothelial cancer. HR (95% confidence interval [CI]) for pembrolizumab and chemotherapy vs. chemotherapy was only 0.78 (0.65–0.93, p=0.0033) for PFS and 0.86 (0.72–1.02, p=0.0407) for OS but, unfortunately, these results were not significant for OS and PFS [54]. PD-1 or PDL-1 inhibitors in urothelial cancer after palliative treatment seemed to have functional limitations. Recently, in the case of stomach cancer, good results were reported in the CheckMate 649 study that showed capecitabine, oxaliplatin, and nivolumab improved OS and PFS compared with conventional chemotherapy in first-line metastatic stomach cancer treatment (OS: HR, 0.80; p=0.0002; PFS: HR, 0.68; p<0.0001) [55].
2. Combination of targeted therapy
In targeted immunotherapy agents, good results have been reported, especially in kidney cancer. Improvement of OS and PFS with the VEGF inhibitor axitinib and pembrolizumab compared to sunitinib, a first-line metastatic RCC (mRCC) conventional treatment (OS: HR, 0.68; p=0.0003; PFS: HR, 0.71; p<0.001) [56,57]. Similarly, lenvatinib plus pembrolizumab compared to sunitinib in first-line mRCC treatment showed a significant improvement in OS (HR, 0.66; p=0.005) [58]. Another study of nivolumab and cabozantinib vs. sunitinib in palliative first-line mRCC showed good results in palliative first-line mRCC treatment. HR (95% CI) for nivolumab and cabozantinib vs. sunitinib was 0.51 (0.41–0.64, p<0.001) for OS and 0.60 (0.40–0.89, p=0.001) [59]. In endometrial cancer, one of the gynecologic malignancies, targeted agents with immunotherapy have been reported to improve survival compared to conventional chemotherapy. Lenvatinib plus pembrolizumab improved OS compared to doxorubicin and paclitaxel treatment in second-line metastatic endometrial cancer in the Keynote 775 study (HR, 0.56; p<0.0001) [60]. The status of deficient mismatch repair (dMMR) in tumors was investigated in this study, and the study showed that the lenvatinib plus pembrolizumab group improved survival regardless of dMMR. The results of the combination with immunotherapy trials are listed in Table 4. Not only VEGF inhibitors but also other targeted agents including poly ADP-ribose polymerase (PARP) inhibitor and CDK4/6 inhibitor with ICIs have benefited from synergistic PD-1/PD-L1 inhibitors in preclinical and early clinical data [61]. In particular, phase II studies of PARP inhibitors with PD-1/PDL-1 inhibitor combination treatment in ovarian and breast cancer have shown positive results, and the results of ongoing randomized control trials will be expected [62-64].
Conclusion
Since 2015, immunotherapy, especially ICI, has become a mainstream cancer treatment. The studies of ICIs showed good responses of various tumor types when applied to many types of cancer. Immunotherapy has a durable response and low toxicity, but immunotherapy alone has a response of 15% to 20% in the cancer patient treatment group. Thus, the challenge of improving the response to immunotherapy was sustained, and we found that the microenvironment in immune cells is very important to act appropriately in cancer. A combination of chemotherapy or targeted therapy with immunotherapy was started on cancer treatment to make an inflamed tumor help increase the response to immunotherapy. Recently, studies on combination therapy reported improved OS and PFS, even though they did not respond to immunotherapy. Many trials of combination therapy are ongoing and will be expected to continue the benefits of survival (Table 5). Thus, combining chemotherapy or targeted agents with immunotherapy is one of the leading pathways for cancer treatment.
Notes
Conflicts of interest
No potential conflict of interest relevant to this article was reported.