Porokeratosis ptychotropica: a case report
Article information
Abstract
Porokeratosis ptychotropica is an uncommon form of porokeratosis, which was initially described in 1995. It is clinically characterized by symmetrical reddish to brown-colored hyperkeratotic, verrucous, or psoriasiform plaques on the perianal and gluteal regions. The lesions tend to integrate and expand centrally, with small peripheral satellite lesions. Early skin biopsy and appropriate diagnosis are essential because malignant change occurs in 7.5% of porokeratotic lesions. Conventional treatment options include topical steroid, retinoid, imiquimod, 5-fluorouracil, isotretinoin, excimer laser, photodynamic therapy, intralesional steroid or bleomycin injection, cryotherapy, carbon dioxide (CO2) laser, and dermatome and excision, but none seem to achieve complete clearance. A 68-year-old woman presented with diffuse hyperkeratotic scaly lichenoid plaques on the buttocks that had persisted for several years. A skin biopsy of the buttocks revealed multiple cornoid lamellae and intense hyperkeratosis. There were some dyskeratotic cells beneath the cornoid lamellae and the granular layer was absent. Porokeratosis ptychotropica was diagnosed based on the characteristic clinical appearance and typical histopathological manifestations. She was treated with a CO2 laser in one session and topical application of urea and imiquimod cream for 1 month. The lesions slightly improved at the 1-month follow-up. We herein present a rare case of porokeratosis ptychotropica.
Introduction
Porokeratosis ptychotropica was initially described in 1995; it is an uncommon form of porokeratosis with a special predisposition to affect body folds [1]. Porokeratosis ptychotropica is clinically characterized by symmetrical reddish to brown-colored hyperkeratotic, verrucous, or psoriasiform plaques on the perianal and gluteal regions. The lesions tend to coalesce and expand centrally, with small peripheral satellite lesions. This is sometimes described as butterfly-shaped appearance [2,3]. Currently, there is no standard treatment for porokeratosis ptychotropica. We report a rare form of porokeratosis that was treated with a carbon dioxide (CO2) laser and topical imiquimod application.
Case
Ethical statements: This study was exempted from review by the Institutional Review Board (IRB) of Keimyung University Dongsan Medical Center (IRB No: 2022-09-012). Written informed consent was obtained from the patient for publication of this case report and any accompanying images.
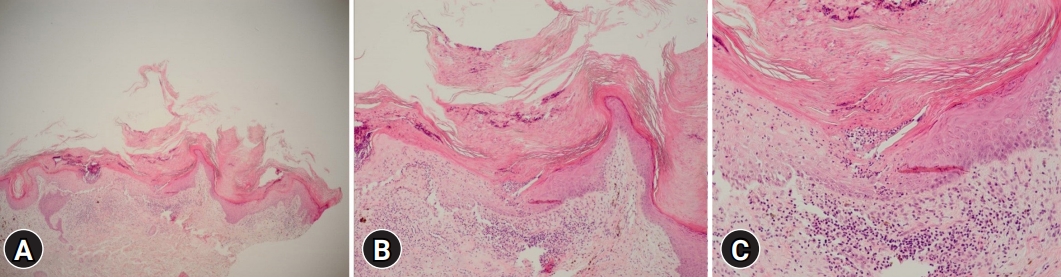
A 68-year-old female patient presented with diffuse hyperkeratotic scaly lichenoid plaques on the buttock that had persisted for several years (Fig. 1A). She had a history of hypertension, chronic kidney disease, heart failure, and hypothyroidism, but no family history of a similar skin lesion. A skin biopsy of the buttocks revealed multiple cornoid lamellae and intense hyperkeratosis (Fig. 2A). There were some dyskeratotic cells under the cornoid lamellae, and the granular layer was absent (Fig. 2B). A diagnosis of porokeratosis ptychotropica was based on the characteristic clinical appearance and typical histopathological manifestations. She was treated with a CO2 laser in one session and topical application of urea and imiquimod cream for 1 month. The lesion thickness and scale slightly improved and the number of satellite lesions was reduced at the 1-month follow-up appointment (Fig. 1B). She denied further treatment because her general condition related to her medical history had worsened.
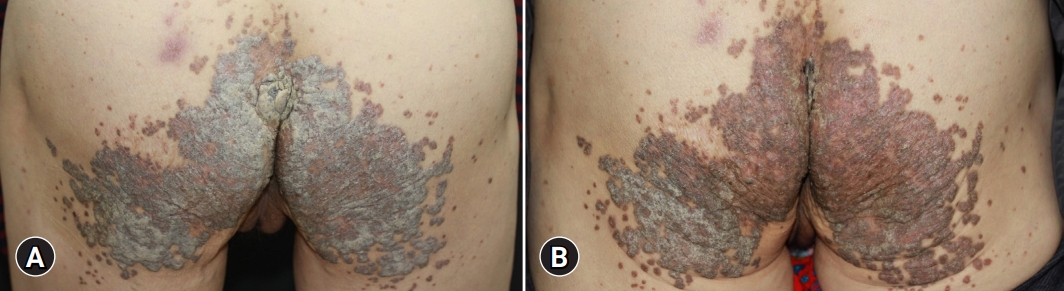
(A) Asymptomatic diffuse hyperkeratotic scaly lichenoid plaques on the buttock that had persisted for several years. (B) The lesions are slightly improved at the 1-month follow-up.
Discussion
Porokeratosis ptychotropica is a rare disease and can mimic viral warts, inverse psoriasis, chronic contact dermatitis, dermatophytosis, candidiasis, squamous cell carcinoma, and condyloma acuminata [4,5]. When encountering an adult with slowly progressing hyperkeratotic verrucous plaques on the buttocks, which had responded poorly to previous treatments, porokeratosis ptychotropica should be considered.
The exact etiology and predisposing factors are unclear. It appears the most reported cases have arisen sporadically [2]. However, as with the classic type of porokeratosis, multiple factors such as ultraviolet light exposure, chronic renal failure, hepatic failure, hepatitis C infection, human immunodeficiency virus infection, organ transplantation, prior chemotherapy, and other immunosuppression-related disorders could be associated with the disease [3].
Skin biopsy is important for an accurate diagnosis and exclusion of other conditions. The histopathological characteristics of porokeratosis ptychotropica do not remarkably differ from those of other porokeratosis variants, including hyperkeratosis of the epidermis, multiple cornoid lamellae in the stratum corneum, focal hypogranulosis, and dyskeratotic cells beneath the parakeratosis. The important feature that distinguishes porokeratosis ptychotropica from typical cases is that in the classic variants, the cornoid lamellae are typically located at the periphery, whereas in porokeratosis ptychotropica, the cornoid lamellae are observed throughout the lesion [3,4].
Malignant transformation occurs in 7.5% of porokeratotic lesions. It is common in large, long-standing lesions and the linear subtype [4]. There is a reported case of development of invasive squamous cell carcinoma in a porokeratosis ptychotropica lesion, and this malignant transformation occurred 18 years after diagnosis of the porokeratosis ptychotropica [6]. Therefore, long-term follow-up of porokeratosis ptychotropica seems important considering its chronic nature, large size, and potential for malignant transformation [4,6].
There are no established treatment alternatives for porokeratosis ptychotropica [7,8]. Conventional treatment options include topical steroid, retinoid, imiquimod, 5-fluorouracil, isotretinoin, excimer laser, photodynamic therapy, intralesional steroid or bleomycin injection, cryotherapy, CO2 laser, and dermatome and excision. None of these options seems to achieve complete clearance [9,10].
There are only three reports of porokeratosis ptychotropica in the Korean literature [11-13], and 45 cases have been reported in the dermatologic literature. Therefore, in this case report, we attempted to highlight the awareness of this condition and emphasize that clinicians should consider porokeratosis ptychotropica in their differential diagnosis when encountering pruritic eruptions in the gluteal regions. Early skin biopsy and appropriate diagnosis are essential because long-term monitoring of such patients is warranted, considering the potential malignant transformation of these lesions [10].
Notes
Conflicts of interest
No potential conflict of interest relevant to this article was reported.
Funding
None.
Author contributions
Conceptualization: all authors; Data curation: YK, JMY, SAK; Formal analysis: YK, SAK; Methodology: YWR; Resources: YWR, YK; Software: YK, JMY; Supervision: SAK; Validation: YWR, SAK; Writing-original draft: YK, JMY; Writing-review & editing: YWR, YK.